Hypoglossal nerve stimulator
Approved in the US in 2014, the hypoglossal nerve stimulator (HGNS) is a second-line therapy for moderate to severe OSA in adults who are unable to tolerate or have failed PAP therapy, in those with AHIs in the 15-65 events per hour range and BMI <32-35 kg/m2. The implanted neurostimulator stimulates the hypoglossal nerve at initiation of inspiration, causing tongue anterior protrusion and stiffening to reduce upper airway collapse during sleep.
Multiple studies show a significant reduction in AHI and oxygen desaturations, as well as improved QoL. For example, the Inspire device, the most widely studied and FDA-approved system, reduces AHI by approximately 20 AHI events per hour in the short-term follow-up (<1 year) and approximately 16 AHI events per hour in long-term follow-up.10 These benefits are durable, with sustained efficacy reported five years after implantation.11
Research continues on alternative approaches to expand eligibility (e.g., higher BMI, alternative pathways of airway collapse). Adverse effects are uncommon and may include tongue discomfort, insomnia, frequent awakenings, and local pain triggered by the stimulation impulse. Despite these issues, adherence and patient satisfaction remain high.
Glucagon-like peptide-1 agonist
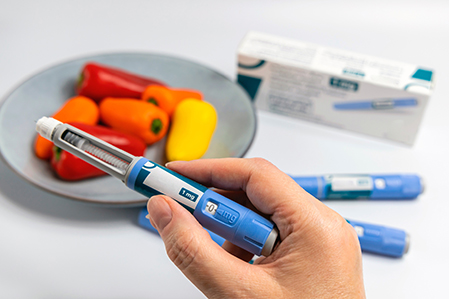
Tirzepatide is the first FDA-approved treatment for moderate to severe OSA in adults with obesity, based on evidence showing substantial reductions in AHI and improvements in patient-reported outcomes and cardiometabolic risk factors. Its efficacy is attributed primarily to weight loss. Studies showed a statistically significant reduction in AHI at 29.3 events per hour compared to a reduction of 5.5 events per hour in the placebo group.12 There were reductions in oxygen desaturation, body weight, systolic blood pressure, and patient-reported sleep symptoms. More than 50% of patients reached AHI thresholds where PAP therapy may no longer be indicated.
In addition to the above results, a study in Chest assessed obese patients with OSA, with the primary outcome of all-cause mortality and secondary outcomes including major adverse cardiovascular events (MACE) and major adverse kidney events (MAKE). Among the 42,300 studied over a nearly three-year period (January 2022 to November 2024), those treated with tirzepatide had a lower risk of all-cause mortality (HR 0.443) compared to placebo, with reduced risks of MACE (HR 0.731) and MAKE (HR 0.427) across all subgroups (age, sex, BMI, PAP use) except for age 18-39. Authors concluded that “tirzepatide may be a potential therapeutic option for improving clinical outcomes [in obese patients with OSA]”.13
While potentially exciting, critics of the study noted that it included significantly obese subjects (BMI >39) and had extensive exclusion criteria, which may limit generalizability. Long-term studies are needed to confirm durability and safety.14
Conclusion
Obstructive sleep apnea (OSA) is a common sleep-related breathing disorder characterized by repeated episodes of partial or complete upper airway obstruction during sleep. Severe, untreated OSA is strongly associated with increased all-cause and cardiovascular mortality.
Although observational studies suggest that treatment may reduce these risks, randomized controlled trials have not yet confirmed a definitive mortality benefit. Current therapies focus on maintaining airway patency, improving sleep quality, and mitigating long-term health risks. Emerging treatments, such as tirzepatide, show promise for reducing mortality, but further research is needed.
For life and disability insurance underwriting, OSA severity, treatment adherence, and comorbidities should be carefully evaluated. As new therapies and stronger outcome data become available, underwriting guidelines are likely to evolve to reflect the complex relationship between OSA management and long-term risk.
RGA experts are eager to engage with clients to better understand and tackle the industry’s most pressing challenges together. Contact us to learn more about RGA's capabilities, resources, and solutions.







