Vaccines save lives. They also end fear. Many still recall the terrifying iron lungs and leg braces from polio or the mid-century wave of rubella that took the lives of many infants. Long before the current pandemic, vaccines have proven to be historical game-changers in the prevention of infectious diseases. RGA sat down with Senior Vice President and Head of Global Medical Dr. Daniel Zimmerman and Global Medical Researcher Hilary Henly to discuss the past and future of vaccination, vaccine hesitancy and equity, and how insurers can help.
How have vaccines impacted the health of humanity over the years?
The development of prophylactic and therapeutic vaccines since the late 18th century has been profoundly instrumental in preventing and containing infectious diseases around the world. The World Health Organization (WHO) declared smallpox officially eradicated in 1980 solely because of vaccination. In 1980, only 3% of one-year old children had been immunized against rubella and 15% against tuberculosis (TB) globally but by 2019, these figures had risen to 71% and 88% respectively.1
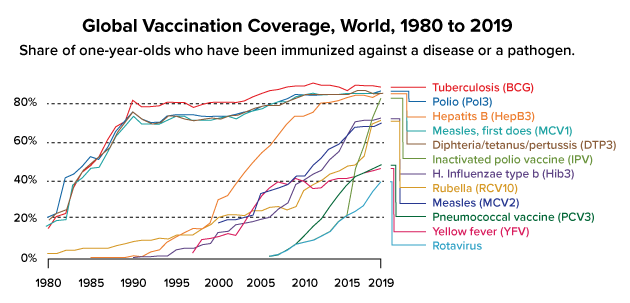
Adapted from World Health Organization (WHO), UNICEF
Vaccines have prevented millions of childhood illnesses and deaths from infections including chickenpox, measles, rubella, TB, and whooping cough and prevented further illness and death from cholera, diphtheria, tetanus and typhoid fever in developed countries where vaccination programs are in operation.2 Immunization has reduced global deaths from measles by 73% between 2000 and 2018, resulting in an estimated 23.2 million fewer deaths.3
What’s new or different about the emerging technologies being used to bring us next-generation vaccines?
Historically, vaccines were created using inactivated viruses (such as one type of polio vaccine) or live-attenuated viruses (yellow fever vaccine). The rapid development of messenger ribonucleic acid (mRNA) vaccines for SARS-CoV-2 was based on years of research and has given real hope to new vaccines being developed for other viruses and pathogens. mRNA is a set of genetic instructions given to cells in order to make proteins, which then trigger an immune response and protects against further infection. They can be rapidly produced, adapted to address mutations, and are cheap to manufacture and relatively easy to administer. mRNA vaccine technology has huge potential to improve human health and positively impact mortality around the world.4
Why are some people concerned about the use of vaccines?
Most medical interventions come with some risk and vaccines are no different. The question is whether the risk, which is usually extremely small, outweighs or is disproportionate to the potential benefits. People view the scale of these risks differently, and misperceptions can lead to vaccine hesitancy.
The other issue has to do with access to vaccine information and misinformation from a wide range of sources, which influence vaccine decision-making. Anecdotal, partial and inaccurate information contributes to misperceptions that can influence vaccine acceptance. Importantly, a lack of trust has contributed to the so-called vaccine-confidence gap.5 Much has been written recently to address vaccine hesitancy through non-confrontational means and by promoting partnerships between health care providers and vaccine-hesitant parents and patients.6
What are some of the issues regarding equitable distribution and access to vaccines for all the world’s citizens?
Facilitating access to safe and effective vaccines in all countries, particularly those where incidence of preventable diseases is high, will help to reduce health inequalities and significantly reduce early mortality. However, low- and middle-income countries often have less access than wealthier nations to vaccines, as high-income countries place large advance orders to purchase any available vaccine supplies. In an effort to ensure supply of COVID-19 vaccines to lower income nations, COVID-19 Vaccines Global Access, known as ‘COVAX’, a global initiative to ensure equitable access to tests, treatments and vaccines for COVID-19, is designed to bring countries together to pool resources and support the development, manufacture, and distribution of vaccines to countries who might otherwise be unable to purchase them.7
How can our industry highlight that vaccine use is of vital interest to all of society and reaffirm the insurance industry’s role in promoting greater understanding of vaccine science?
Vaccines generally have an excellent safety record and go through multiple tests and trials before being finally approved (or rejected) for use in the general population. Many published scientific studies and national strategies have demonstrated the beneficial effects of vaccines. For example, vaccination programs in the U.S. for diphtheria, Haemophilus influenzae type b (Hib), hepatitis B, human papillomavirus (HPV), measles, mumps, pertussis (whooping cough), polio, rubella, tetanus and varicella prevented an estimated 20 million infections and 12,000 deaths and permanent disabilities in 2014.8
The insurance industry can help contribute to public understanding of the benefits of vaccination by discussing the health effects of vaccines, addressing misconceptions, and presenting scientific facts in a way that is easy for the general public to interpret, allowing them to understand the health benefits and importance of vaccination and make more informed decisions.