Population demographics are changing with the net result being an increasing number of aging individuals with a wide variety of needs around insurance and wealth transfer.
In 2014, 14.5% of the US population was age 65 or older (46.3 million people). This is expected to increase to 23.5% of the population by the year 2060 (98 million people).
1 Accompanying these demographic changes are biomedical advances and public health policies that improve life expectancy. Epidemiologic changes have shifted the disease burden toward a pattern of multiple chronic diseases with aging. Notable changes in the top 10 causes of death in individuals over 65 years of age from 2000 to 2018 have occurred, with Alzheimer’s dementia and unintentional injuries moving up the list. This exemplifies the importance of understanding frailty, a common co-morbid condition to dementia.
1
According to a recent SOA survey, 70 is the most common age used to define the older age market. Challenges in underwriting this market include:
- Poor correlation between age and function.
- Functional capacity, as measured by both mental and physical activities, is rarely described in an APS.
- Cognitive screening is helpful to identify a potential problem but usually lacks the necessary context to be truly accurate.
- Changes in health or functional status are inconsistently documented and investigated.
Figure 1 (next page) illustrates the complexity of the typical geriatric patient; multiple co-morbid conditions are common with increasing age. The percentage of the population with hypertension, asthma, COPD, diabetes and cancer has risen since the late 1990s.1
To underwrite aging individuals, it is essential to con- sider the unique aspects of the cohort. Geriatricians identify delirium, frailty, dementia, falls and urinary incontinence as geriatric syndromes. These conditions negatively influence long-term outcomes. There are interventions that improve functional status and improve long-term outcomes, but the presence of a geriatric syndrome must first be identified.
Figure 1. Percentage of People Age 65 and Over Who Reported Having Selected Chronic Health Conditions, By Sex, 2018
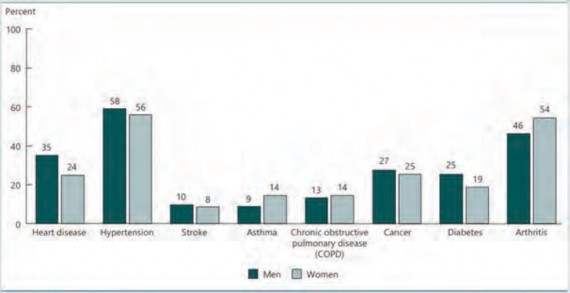
Note: Chronic obstructive pulmonary disease (COPD) is defined as responding yes to questions on ever having emphysema, COPD, or having chronic bronchitis in the past 12 months. This definition has changed from previous editions of Older Americans. Reference population: These data refer to the civilian noninstitutionalized population.
Source: National Center for Health Statistics, National Health Interview Survey. https://agingstats.gov/docs/LatestReport/OA20_508_10142020.pdf
Frailty may underlie several of the other geriatric syndromes. This article will address the definition and prevalence rates of frailty, and describe one of the most widely used frailty scales in geriatric research, providing proxies for the information. The article will also discuss two cases that illustrate information reflective of a frail applicant and describe the influence of COVID-19 on frailty, based on data gathered over the last year.
Defining and Understanding Frailty
Frailty is often defined as a syndrome that leads to lack of physiologic reserve and vulnerability to either external or internal insult, ultimately leading to poor outcomes with increased mortality risk. Frailty is more common with increasing age and is difficult to identify because it is not a discrete medical condition but may involve multiple organ systems. It exists on a spectrum of disease ranging from pre-clinical to severe disease and is commonly associated with cognitive decline, depression and worsening functional capacity.
Studies evaluating frailty in community-dwelling individuals over age 65 report a prevalence of 4-16%2 and up to 43% in those diagnosed with cancer.3 Another population at high risk for frailty is the nursing home population, with prevalence rates as high as 52% noted in a large meta-analysis published in 2015. Fried et al.4 looked at 4-year age bands, beginning at age 65 and ending at age 90+, and found increasing prevalence rates of frailty in older age groups and in women. One explanation for the increased prevalence in women is related to sarcopenia, leading to generalized weakness and susceptibility to functional decline.2
Table 1. Prevalence of Frailty at Baseline in the Cardiovascular Health Study, Original Cohort (1989-1990).
Age (In Years) | N /span> | Overall
% Frail | Women (n=2,710)
% Frail | Men (n=2,025)
% Frail |
|---|
65-70 | 2,308 | 3.2 | 3.0 | 1.6 |
|---|
71-74 | 1,271 | 5.3 | 6.7 | 2.9 |
|---|
75-79 | 1,057 | 9.5 | 11.5 | 5.5 |
|---|
80-84 | 490 | 16.3 | 16.3 | 14.2 |
|---|
85-89 | 152 | 25.7 | 31.3 | 15.5 |
|---|
90+ | 39 | 23.1 | 12.5 | 36.8 |
|---|
Total | 5,317 | 6.9 | 7.3 | 4.9 |
|---|
Source: Adapted from Fried et al. Figure 4, p. M151.
Assessment of Frailty/Screening Tools
There are a multitude of different screening tools for frailty; however, not all contain information that can be applied to the information we may receive in the application and underwriting process of an elderly applicant which can provide meaningful data to risk assessment.
Frailty is typically multifactorial. Components that commonly contribute to frailty include: unintentional weight loss, low levels of physical activity, weakness, poor endurance, exhaustion, depression, cognitive impairment, co-morbid conditions and polypharmacy.
The Fried Phenotype
Linda Fried, M.D., and colleagues published one of the hallmark articles on the topic titled “Frailty in Older Adults: Evidence for a Phenotype,” which describes clinical criteria to identify the syndrome of frailty.2 This important body of research was written to standardize a definition for frailty and demonstrate predictive value for various outcomes, including:
- Incident disease
- Hospitalization
- Falls
- Death
Fried’s phenotype of frailty includes three or more of the criteria discussed below. Those who are considered at high risk to develop frailty, called pre-frailty, must have one or two criteria present:
1. Unintentional weight loss, poor appetite and malnutrition: Unintentional weight loss of over 10 pounds in the last 12 months or over 5% of total body weight in the last 12 months.
- The best markers for malnutrition in insurance labs are cholesterol and albumin.
- BMI is not a good marker for malnutrition in obesity. (With age, lean mass decreases and fat mass increases.)
2. Weakness: Weakness is tested by grip strength. While grip strength is not measured in clinical practice very often, it is an important proxy for lean body mass. Strength is important for maintaining independence. It requires strength to perform activities of daily living (ADLs) and instrumental activities of daily living (IADLs). Poor oral intake, inactivity and depression may all be the root cause for developing weakness. Proxies for weakness may be the inability to perform or delay in performing certain IADLs. Sample IADL.
- Light housekeeping chores require 1.5-4.0 METS (metabolic equivalents).5
- Examples include: Making the bed, vacuuming carpet, washing dishes and food preparation.
- Timed get up and go test (TGUG) measures the time to get up from a chair, not using hands, walk 10 feet, turn around and return to the seat. Assistive devices may be used. This test is often seen as part of insurance applications for older age applicants. There is risk for frailty, falls and imbalance with abnormally delayed TGUG.6,7,8
- Heavy housekeeping requires 3.5-5.0 METS.
- Other examples include: Mopping floors, mowing the lawn (riding mower), raking leaves.
3. Exhaustion: Exhaustion is measured by questions from the Center for Epidemiological Studies Depression Scale (CES-D) to measure psychologic well-being and/or depression on a continuum scale. Depressive responses suggest a higher probability of depression along with other co-morbid conditions, such as frailty or IADL dependence.9
4. Poor endurance and energy/exercise tolerance: Physical activity is inversely associated with mortality from cardiovascular disease and malignancies. Myers and colleagues10 demonstrated the association between METS achieved on a stress test and mortality. The risk is increased substantially at < 5 METS on stress testing. Intermediate risk is noted with 5-8 METS, and the most favorable mortality is associated with exercise capacity above these levels. Exercise capacity and physical activity have both been shown to correlate with survival in other large cohort studies.
5. Low activity: Frequency and duration of exercise may be established by simple questions such as: “Are you able to walk a block without stopping, mow the yard, rake the yard, garden and do any type of regular fitness activity?” Inability to complete these tasks once to twice a week means activity is abnormal.
Table 2. Timed Get Up and Go (TGUG) Cut-Off Scores Vary by Source and Population
Population | Cut-off (seconds) | Article |
|---|
Community dwelling men, women age 60-69 | 8 (mean) | Staffen et al. 2002 |
Men, women age 70-79 | 9 (mean) | Staffen et al. 2002 |
Men, women age 80-89 | 10 (mean); 11 (mean, women) | Staffen et al. 2002 |
Hip OA | > 10 | Arnold et al. 2007 |
Frail elderly | > 32.6 | Thomas et al. 2005 |
Source: Adapted from slide – Original reference unknown.
Figure 2. Exercise Capacity and Mortality
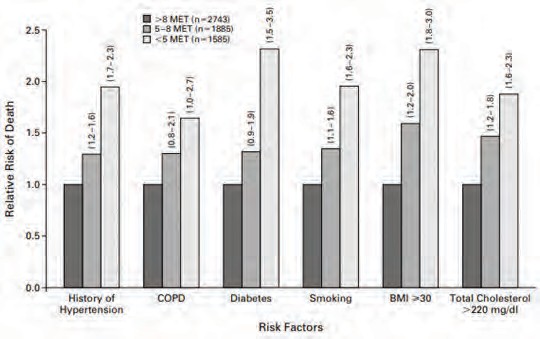
Note: Relative risks of death from any cause among subjects with various risk factors who achieved an exercise capacity of less than 5 MET or 5 to 8 MET, as compared with subjects whose exercise capacity was more than 8 MET. Numbers in parentheses are 95% confidence intervals for the relative risks. BMI denotes body-mass index, and COPD denotes chronic obstructive pulmonary disease.
Source: Jonathan Myers, PhD, Manish Prakash, MD, Victor Froelicher, MD, Exercise Capacity and Mortality Among Men Referred for Exercise Testing. N Engl J Med 2002; 346:793-801 DOI: 10.1056/NEJMoa011858.
Frailty and COVID-19 Infection
Frailty is defined as a lack of physiologic reserve, including reduced immune function. Therefore, identifying an individual with both COVID-19 infection and frailty predicts a poor outcome. In a meta-analysis of 16 cohort studies including over 4,000 patients, Yang and colleagues11 looked at the impact of frailty on COVID-19 outcomes. Not surprisingly, they found frailty was associated with increased all- cause mortality in patients with COVID-19 (OR=1.81, 95%CI:1.48-2.21). This was consistent across patient age, patient source and definition of frailty. Frailty was also associated with more severe COVID-19, ICU admission, mechanical ventilation and longer length of hospital stay. Identification of frailty in those infected with COVID-19 may improve medical management and resource allocation during the pandemic where medical assets are scarce.
Conclusion
- Frailty is one of the geriatric syndromes and should be considered when underwriting anyone 70 years or older.
- Frailty is multifactorial and increases the risk for poor outcomes including death.
- Co-morbid conditions commonly associated with frailty include: cognitive impairment, depression and polypharmacy.
- Fried identified five markers for frailty; at least three must be present to diagnose frailty and one or two present for pre-frailty or high risk for frailty:
- Unintentional weight loss (10 pounds).
- Weakness
- Exhaustion (may be a manifestation of depression).
- Poor endurance and low energy
- Low activity.
Sample Case Studies
Case Study 1
70-year-old female. History of diabetes, hypertension, former smoker (quit 5 years ago).
Current height and weight from exam: 5’5” 126 pounds; weight from 2 years ago was 150 pounds.
Labs: A1C=%6.3, Albumin=4
Medical records: The last office visit in March 2021 noted complaints of anxiety, depression and lack of energy during the COVID-19 time period. Patient admitted her spouse has been having to complete her past duties of cooking and cleaning the house. She has started sleeping late. When questioned further, she says she goes to bed at 9:00 p.m. and gets out of bed around 11:00 a.m. Her prior year physical in 2019 noted weight was 150 pounds. Timed get up and go: 17 seconds; delayed word recall: 6/10.
Relevant factors for frailty: change in weight, depression/anxiety, inability to perform some IADLs (change in functional status) and delayed TGUG.
Positive factors: Normal serum albumin, well-controlled diabetes, acceptable DWR performance.
Conclusion: PI has multiple factors suggesting frailty: weight loss, fatigue, depression, dependence in some IADLs. Using the Fried criteria, the PI has at least three factors that suggest frailty.
Case Study 2
72-year-old female. 5’ 3” 170 pounds. History: No admitted health concerns; noted recent CPE with mammogram normal.
Medical records: One office visit in February 2021 noted health history of hypertension and fatigue. CBC and all other labs normal. Senior supplements all cognitive testing normal. Timed get up and go: 45 seconds.
Very limited APS records were sent. The PI had lost her husband 8 months prior to application for insurance, had experienced some mild depression, and had been prescribed low-dose citalopram with improvement in symptoms. Despite the intact cognitive testing, the examiner had made a comment that the PI had trouble getting out of her chair to perform the timed get up and go test (TGUG).
Conclusion: PI appears pre-frail due to the delayed TGUG and difficulty with rising from a chair. Fatigue mentioned in the comments may be related to depression, but she is under treatment for depression and appears to be doing well. Using the Fried criteria, PI appears to be pre-frail. Present are both fatigue and delayed TGUG.
Favorable factors include treatment of depression with good response to antidepressant medication. Consider insuring since cognitive testing and physical parameters are stable.
Innovations across the insurance industry are helping to improve risk insights. It is never too early to start educating yourself and engaging with a partner.