Diabetes is a chronic and often debilitating disease defined by the presence of chronic hyperglycemia, due to the body’s inability to produce or process insulin. Its presence increases the risk of numerous complications in the cardiac, renal, ophthalmologic, and nervous systems, resulting in higher mortality rates.1
While clinical literature has extensively identified the risk drivers of mortality of those with diabetes, this article focuses on all-cause mortality experience related to diabetes using non-clinical metrics.
This paper is the first to examine the mortality experience based on databases from both MIB’s impairment records and RGA’s prescription drug history information. MIB and RGA each utilized separate and independent diabetes-related data sources to conduct these analyses.
MIB Databases and Methodology
The MIB established two databases to conduct its analysis. The first, compiled from member company information, consisted of life insurance applicants who indicated in their applications they were found to have diabetes or hyperglycemia. The second, data on deaths, was compiled from the Social Security Administration’s Death Master File, obituaries in newspapers or posted by funeral homes, and state vital records. In total, the MIB’s Other Death Source database had more than 3,000 sources of death notifications.
After transformation, the MIB dataset contained 26,642,845 person-years of exposure and 179,832 all-cause deaths. Exposure was defined as the time in years, from the first report of the presence of diabetes or hyperglycemia to the MIB database (i.e., the impairment report date) until February 2019. If the applicant died before February 2019, the individual’s exposure was considered to be the number of years between the impairment report date and the date of death, rounded up to the next integer.
The 2015 Valuation Basic Table (VBT) select and ultimate (age last birthday) sex-distinct table was used as the expected basis. Since death data tends to be under-reported, the absolute level of actual vs. expected ratios (A/Es) could be understated. However, if we could assume under-reporting of deaths affects different categories in a proportional fashion, relative A/Es could still be meaningful.
RGA Databases and Methodology
For its analysis, RGA also used two datasets. The first was drawn from the prescription drug histories and death information of millions of individuals, from which a cohort of individuals was identified who had used drugs that typically treat diabetes, dating from 2007 to 2014. The second dataset, for the experience study portion, covered mortality experience during calendar years 2015 to 2017 and contained 5.5 million person-years of exposure with approximately 123,000 deaths. The expected basis was the empirical mortality experience of both datasets taken together by attained age, gender, and calendar year.
Experience by Age and Gender
Chart 1 compares RGA and MIB mortality experience data by age. Note that MIB age data used age at application, while the RGA data used attained ages.
Although mortality by age from both studies is close, it is based on two entirely different datasets and different expected bases. Therefore, correlation should be interpreted with caution, given the differences in datasets.
Except for those between the ages of 25 to 40, Chart 1 shows the mortality experience of the RGA group, measured by A/Es, decreases by age. This indicates the mortality gap between diabetes patients and their non-diabetes peers is more pronounced for younger individuals, which is consistent with the clinical literature.
Note: The exception data point, RGA age group 25 to 40, may be less credible as it only contains a few hundred deaths.
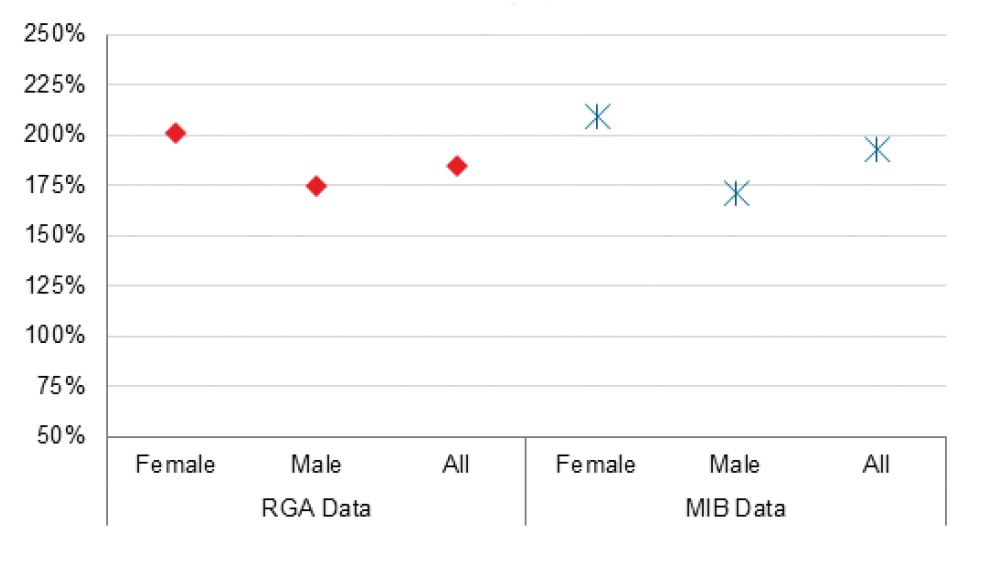
Chart 2 compares mortality experience by gender for the two different datasets.
Both the MIB and RGA data indicate that mortality for females with diabetes is much higher than for males.
Experience by Types of Diabetes
The MIB member company database includes information about diabetes treatments from attending physician statements (APS) and paramedical exams, as well as self-disclosure by the applicants. The information is provided in four categories: diet, oral medications, insulin, and unknown.
Those reporting use of multiple diabetes treatments were categorized by the more severe treatment option. For example, a person using both oral medications and insulin was classified as using only insulin.
Chart 3 illustrates the MIB analysis, which indicates people who take insulin as the most severe treatment have the highest relative mortality experience, followed by those taking oral medications. Among all three treatments, diet is used to treat milder cases of diabetes as evidenced by the lower mortality seen in Chart 3.
The RGA cohort’s data, illustrated in Chart 4, was categorized differently. Individual diabetes prescription drug histories were classified as insulin only, insulin and non-insulin, and non-insulin only.
Individuals with type I diabetes are generally assumed to use only insulin for blood sugar control. According to clinical literature, these individuals may have higher relative mortality than those with Type 2 diabetes. Unlike the MIB result, the attained ages group 25 to 40 were shown to have lower mortality than groups at older ages. However, this finding could be called into question given the relatively low presumed numbers of individuals with type I diabetes.
A person whose treatment is non-insulin only is more likely to represent an individual with Type 2 diabetes on oral medications (the gray line). The analysis showed that particular group had the lowest mortality.
A person using both insulin and non-insulin treatments (the red line) is more likely a Type 2 diabetic with more advanced disease. Their mortality is in between those treated with insulin only and those treated with non-insulin only.
Experience by Time Since Diagnosis
At the time of policy application, MIB collects information about the length of time since a diabetes diagnosis. Chart 5 illustrates A/Es by age at application and time since diagnosis.
In general, according to MIB data, the longer a person has been diagnosed with diabetes, the worse the mortality. It is especially true for younger individuals with diabetes.
Note: The RGA dataset was based on prescription drug histories. There was only reliable information on what treatments were used, and none on when the person was first diagnosed.
Experience by Metformin Adherence
The American Diabetes Association (ADA) and European Association for the Study of Diabetes (EASD) published a consensus report in 2018 showing that the medication metformin is generally the first line of treatment for Type 2 diabetes.
When a person takes metformin, the ratio of adherence correlates with the level of mortality. ”Ratio of adherence” is defined as the ratio of the number of days metformin was taken to the total number of days a person was eligible for prescription drug benefits.2
Chart 6a illustrates the experience of people in the RGA cohort who used only non-insulin treatments for their diabetes. As indicated above, these individuals most likely had relatively less advanced Type 2 diabetes without complications. Chart 6b shows mortality for those categorized as using both insulin and non-insulin treatments. They most likely had more advanced Type 2 diabetes, with complications.
In Chart 6a, the lines are largely flat, showing that for less advanced Type 2 diabetes patients, consistently taking metformin marginally improves mortality. The blue line is above the red line showing that for less advanced Type 2 diabetic patients, treatment with multiple non-insulin diabetic drugs was associated with heightened mortality.
Chart 6b represents more advanced Type 2 diabetic patients. As expected, mortality experience for this group is much higher than for those with less advanced diabetes. Both the red and blue lines in that section show decreasing mortality by the adherence ratio. Hence, the more consistently those patients are at taking the metformin, the better the mortality. The red line is above the blue line, meaning that for more advanced Type 2 patients with diabetes, use of multiple non-insulin drugs is associated with lower mortality.
Note: MIB data is based on impairments and does not contain prescription drug details.
Conclusions
Overall, people with diabetes have higher mortality than their peers. The elevated mortality is particularly noticeable for two cohorts: people of younger ages and females. Different treatments likely reflect different types of diabetes, and to some extent, the presence of complications. The results of our analysis indicate the following:
- Type I diabetes, treated with insulin, tends to have the highest mortality
- Individuals with less advanced Type 2 diabetes, treated with non-insulin drugs only, have the lowest mortality
- Prediabetes and mild diabetes treated by diet alone have the lowest mortality
The MIB analysis by time since diagnosis indicates the longer a person has been diagnosed with diabetes, the worse the mortality, a result consistent with the clinical literature.
We hope this article has been illuminating and informative. We believe these insights, along with the research, analytics, and modeling capabilities underpinning them, will ultimately strengthen and enrich our industry’s underwriting capabilities.