Colorectal cancer (CRC), while common in terms of incidence and mortality, had historically been a cancer of older adults; however, cases in individuals ages 50 and younger are on the rise.
This has led to recommendations that surveillance begin earlier. Additionally, prognoses in younger individuals may not be as favorable as those diagnosed later in life. Underwriters must start paying more attention to symptoms in younger individuals.
Background and epidemiology of colon cancer
Colorectal cancer (CRC) is a common cancer. It is the third most frequently diagnosed cancer in the US and the third leading cause of mortality for both men and women. It is estimated that in 2020, there were more than 104,000 newly diagnosed cases of colon cancer and 43,000 cases of rectal cancer in the US, and more than 53,000 related deaths. While the majority of cases are diagnosed in individuals over age 50, the proportion of cases in younger individuals increased from 6% in 1990 to 11% in 2013. Mortality for those presenting with colon cancer over the age of 50 has been declining; however, it has been increasing in those under age 50.[1,2] There are multiple theories as to what is causing the rise in cases of CRC in younger adults. Some risk factors have become more common, such as obesity and physical inactivity. However, other theories point more to changes in diet and gut bacteria (gut microbiome) affecting inflammation or immunity in the GI system. Additionally, exposure to elements in the environment, such as air or water pollution or pesticides, may directly or indirectly affect individuals beginning in the womb.[3] Research into increasing cases in younger individuals is ongoing. Currently, there are many known risk factors for CRC, both modifiable and nonmodifiable.[2]
Modifiable Risk Factors | Nonmodifiable Risk Factors |
|---|
Overweight/obesity Physical inactivity Diet - High: red meat, processed meat
- Low: dairy, calcium, fiber (?)
Smoking Heavy alcohol use | Older age Medical history: - Polyps
- IBD
- Family history CRC/adenomatous polyps
- Familial/inherited syndromes
Race/ethnicity Type 2 diabetes Radiation to abdomen/pelvis |
Etiology
CRC almost always begins as a polyp in the mucosa layer of the colon/rectum and follows a consistent sequence from normal mucosa to adenomatous polyp to dysplasia and finally to invasive carcinoma. Different types of changes can occur in colonic mucosa along this path. Some genetic changes allow for “gain of function,” allowing cells to behave in abnormal ways. Other changes inhibit normal genetic function, such as the silencing of repair genes. One such change leads to the accumulation of abnormal short sequences of DNA called microsatellites and a condition called “microsatellite instability.” Finally, epigenetic changes can also alter gene function in deleterious ways.[4,5]
Seventy percent of CRC case are sporadic. About 25% are known to be familial with unclear genetics, and about 5% are associated with specific syndromes caused by germline mutations. Some of the germline syndromes are associated with polyps and others are not. Those associated with polyps include familial adenomatous polyposis (FAP), MUTYH-associated polyposis (MAP), Peutz-Jeghers, juvenile polyposis, and PTEN hamartoma tumor syndrome. Hereditary nonpolyposis CRC/Lynch syndrome is the most common syndrome without polyps. Several of these syndromes are also associated with increased risk for other types of cancer.[4,5]
Colon Polyps
Polyps are found in about half of average-risk 50-year-olds undergoing colonoscopy; however, less than 10% progress to invasive cancer. Polyps are also more common in older individuals and in men. Progression from polyp to cancer is slow, taking 10- 20 years.[6,7]
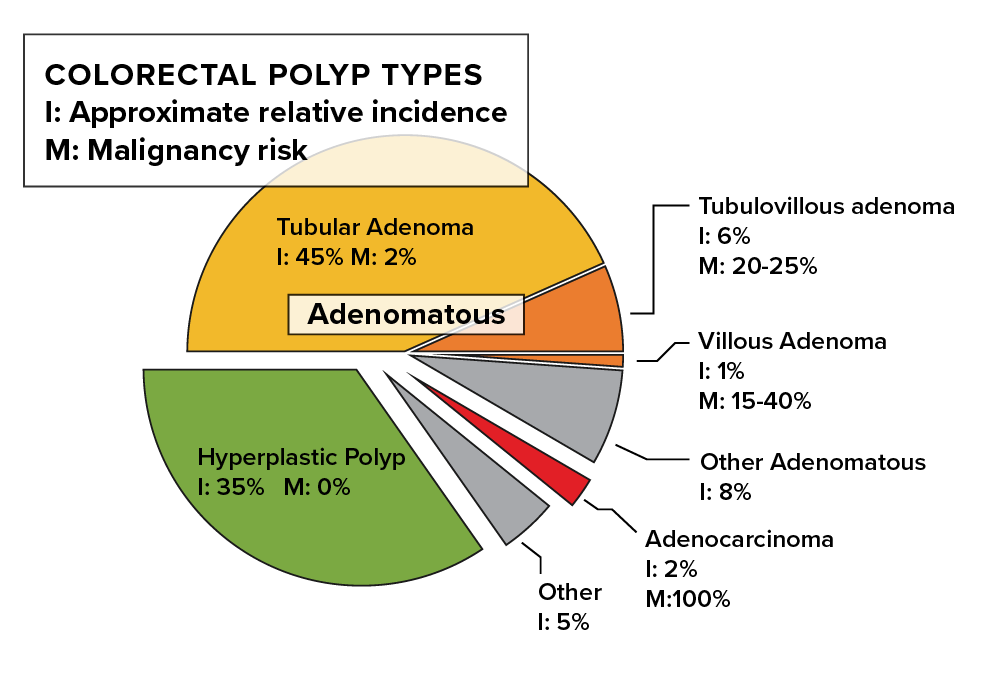
Different types of polyps carry different risk for progression to invasive cancer.[6,7] (see table below)
By the time symptoms develop in CRC, disease is often advanced. Common symptoms include:
- Change in bowel habits: diarrhea or constipation, change in stool caliber or consistency, or feeling of incomplete evacuation.
- Rectal bleeding or blood in the stool.
- Abdominal discomfort – cramps, gas, pain.
- Advanced – fatigue, weakness, unexplained anemia or weight loss.[2]
Polyp Type | Description | Risk or Progression to Cancer |
|---|
Inflammatory | - Usually seen in inflammatory bowel disease (IBD)
- May also be called pseudopolyp
- Not true neoplastic polyp
| Low risk (although there is an overall increased risk of CRC in those with IBD) |
Hyperplastic | - Most common non-neoplastic polyp in colon
- Typically small
| Low risk |
Adenomatous | - About 70% of polyps are adenomatous
- 80% of adenomatous polyps are tubular
- Villous and tubulovillous adenomas are less common
| Increased risk. Risk higher with: - Larger polyps
- High grade dysplasia
- Villous or tubulovillous histology
|
Traditional Serrated Sessile Serrated | - Smooth surface, may be hard to detect
- Often have high-grade dysplasia
| Increased risk |
Source: https://healthblog.uofmhealth.org/digestive-health/a-colon-polyp-primer-know-types-and-your-risk-factors.[7]
In individuals without symptoms, most polyps are identified during routine screening. Currently in the US, the US Preventative Services Task Force and American College of Gastroenterology recommend that adults ages 45-75 years are screened for CRC.[8,9] Different guidance may be recommended for those who are at above-average risk. Globally, most highincome countries recommend screening by age 50 in average-risk individuals.[10] In the US, screening tests may include stool tests (gFOBT, FIT or FITDNA), flexible sigmoidoscopy, colonoscopy or CT colonoscopy.[11] Each of these has a different follow-up recommendation depending upon test outcome and personal risk profile. The colonoscopy has the highest detection rate of all the CRC screening tests and has shown effectiveness, across a range of studies, in decreasing both incidence of CRC and mortality from CRC.[9]
Staging and treatment
Clinically, CRC is staged using the American Joint Committee on Cancer (AJCC) TNM system.[12] The T or “tumor” component refers to the size of the tumor and whether it has invaded the colon/rectum wall. The N or “node” component refers to whether regional nodes are affected. Finally, the M or “metastasis” component refers to whether there is spread to any distant sites. Staging includes both a clinical and pathological system. Clinical staging uses any information that is obtained prior to surgery including physical exam, biopsies and imaging. This is less accurate than the pathological staging, which is obtained from post-surgery pathology reports. Whenever possible, pathological staging should be used for underwriting. An older system of staging, called Dukes staging, is a system of pathological staging without including lymph nodes or metastases that may occasionally still be seen.[13]
Treatment for CRC depends on location and stage at diagnosis.[14] For colon cancer, surgery to remove the tumor is often the primary treatment. For carcinoma in situ (CIS) and localized cancer, surgical resection, including nearby lymph nodes, may be the definitive treatment. For regional cancers, where lymph nodes are involved, adjuvant chemotherapy may also be recommended. When cancer has spread to distant sites, treatment is primarily palliative and may include surgery, chemotherapy and other targeted therapies when appropriate. Genetic testing of the tumor can identify if it will respond to drugs targeting VEGF or EGRF. Additionally, some CRCs can be treated with immunotherapy.[2]
Rectal cancer is also primarily treated with surgery, but more often, it is additionally accompanied by chemotherapy and radiation. Depending on the extent of the cancer, some patients require a permanent colostomy. For early-stage cancers (CIS and localized), surgery is the primary treatment, either through the anus or via an abdominal incision. When surgery is not possible, radiation is the preferred treatment. Regional stage cancers, which have spread to lymph nodes, often require treatment with chemotherapy and radiation prior to surgery in addition to surgical resection. Treatment for distant-stage rectal cancer is primarily palliative. Like distant-stage colon cancer, it may include surgery, chemotherapy, radiation and additional targeted therapies.[2]
Prognosis
Overall relative survival from CRC is 64% at 5 years and 58% at 10 years; however, this does not take into consideration that prognoses vary greatly by stage at diagnosis.[2] Survival is divided by cancer location in the colon as opposed to the rectum and by stage. At diagnosis of colon cancer, 39% of people are diagnosed with localized disease, which has a 5-year survival rate of 90%, compared to a 71% survival rate at 5 years for those diagnosed with regional disease, and only 14% 5-year survival rate for those diagnosed with distant disease. More patients with rectal cancer are diagnosed with local disease (41%), which has an 89% 5-year survival rate. Regional disease at diagnosis has a 72% 5-year survival rate, and distant disease has a 16% survival rate at 5 years.[2,15]
Conclusions
- Colorectal cancer (CRC) is a common cancer and is increasing in incidence in younger individuals.
- Mortality in younger individuals is greater than in those diagnosed at older ages.
- Underwriters should use pathological staging since surgery is the primary treatment for CRC.
- Polyps are relatively common, but most do not progress to invasive cancer in average-risk individuals.
- Don’t overlook what may appear to be minor symptoms if they are recent (within the last year) or if they seem to be occurring more frequently or closer together than in past history.